
Did you know that one of the most common age-related eye conditions is diabetic retinopathy? You can only develop diabetic retinopathy if you have diabetes.
However, as type 2 diabetes is most common in older individuals, so is diabetic retinopathy. Much like other age-related eye conditions, the eye condition doesn’t present any symptoms in the early stages.
When it does begin to present symptoms, the damage already done to the eyes can be extensive and irreversible. This is why it’s so important to have regular eye exams to detect and treat diabetic retinopathy as early as possible.
It’s also important to be aware of any eye condition you may be in danger of developing. Keep reading to learn more about what diabetic retinopathy is, what some of the early symptoms are, who’s at risk for diabetic retinopathy, and how to treat it.
What is Diabetic Retinopathy?
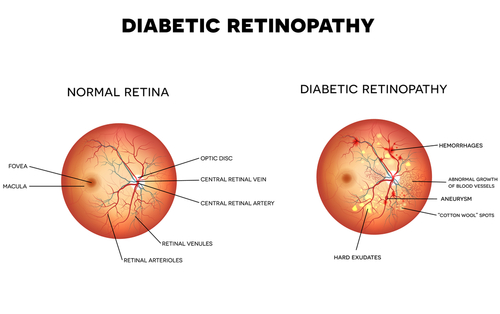
Diabetic retinopathy occurs when blood vessels in the retina grow abnormally, swell, and leak. Abnormal blood vessels in the retina happen when you have consistently high blood sugar.
When these blood vessels swell and leak, it creates scar tissue on the retina. The retina contains photoreceptor cells that translate the light that passes through your eye into impulses sent to the brain.
Scar tissue destroys these photoreceptor cells and damages your vision, as your retina can’t translate a complete picture of what you’re seeing. The difficulty with diabetic retinopathy is it doesn’t present symptoms in its early stages.
When it does present symptoms, those symptoms may never go away. You need an early diagnosis and the soonest possible treatment to prevent vision loss.
Symptoms of Diabetic Retinopathy

When your blood vessels begin to grow and swell, you likely won’t notice it is occurring. They don’t cause any pain or visual issues at first.
Your eye doctor at St. Luke’s at The Villages can see the blood vessels when examining your eyes. But without an eye exam, there’s no way to know if you have diabetic retinopathy if it’s in the early stages.
The first symptoms develop when these blood vessels start leaking into the vitreous. The vitreous is the gel-like fluid inside the eye.
If blood vessels leak into the vitreous, it can cause dark spots in your vision or streaks that look like cobwebs. These symptoms may go away independently as the blood clears, but you need treatment to prevent permanent vision loss.
If left untreated, scarring can cause blurry vision, floaters, blurry and dark spots in your vision, and vision loss. These symptoms usually do not go away, even with treatment, so treatment must be prompt to prevent further damage.
Risk Factors of Diabetic Retinopathy
The primary thing that puts you at risk for diabetic retinopathy is uncontrolled diabetes. But you’re also at higher risk if you:

- Have high cholesterol
- Have high blood pressure
- Use tobacco products
- Are of African, Hispanic, or Native American descent
- Have had diabetes for a long time
Some of these factors can be mitigated to lower your risk. However, some can’t.
If you have diabetes or are at risk for diabetes, you should schedule regular eye exams with your ophthalmologist. Eye exams are the only way to detect diabetic retinopathy early.
You may need more frequent eye exams if you’re at a higher risk for diabetic retinopathy. Your eye doctor can discuss how frequently you need eye exams and determine the best schedule.
Even if you don’t have diabetes, you should have regular eye exams after turning 40. Several age-related eye conditions don’t show early symptoms and can lead to permanent vision loss.
Regular eye exams are vital as you age; they’re usually the only way to know if you need treatment for an eye condition. Be sure to talk to your eye doctor about your risk for diabetic retinopathy and other age-related conditions so they can recommend the best schedule for your eye needs.
Treating Diabetic Retinopathy
Diabetic retinopathy, like diabetes, has no cure. However, with management, some treatments can prevent further vision loss.
At St. Luke’s at The Villages, we offer the following treatments for diabetic retinopathy:
Injections
One way of treating diabetic retinopathy is by injecting medication into the eye. Two kinds of medications do this: Anti-VEGF injections and steroids.
Anti-VEGF injections reduce blood vessel growth by inhibiting the protein that stimulates growth, called anti-vascular endothelial growth factor, or VEGF. Steroid injections reduce swelling in the blood vessels.
Steroid treatment is only used with caution, as extended steroid use can raise your risk for other eye conditions like cataracts. However, depending on how severe your case of diabetic retinopathy is, this risk may be worth the benefits of steroid treatment. Injectable steroids can help reduce macular swelling.
Laser Treatment
There are several different kinds of laser treatment for diabetic retinopathy. These treatments use specialized lasers that target blood vessels to seal them off and shrink them, stopping the leaking into the retina.
These treatments may be used in conjunction with injections to prevent further blood vessel growth.
Vitrectomy
A vitrectomy is a procedure performed to remove part of the vitreous. It’s often done to remove the vitreous gel and blood from leaking vessels in the retina. Sometimes this blood clears on its own, but a vitrectomy can be an effective solution when it doesn’t.
If you’re at risk for diabetic retinopathy, don’t wait until you experience symptoms to see your eye doctor. Schedule an appointment now at St. Luke’s at The Villages in Lake Sumter Landing, FL, to take control of your vision!









